Loading Printer-friendly page
This information has been compiled from multiple sources.
Basic Information about Lyme Disease
 |
Lyme Disease was first recognized in the United States in 1975 by Dr. Allen Steere, following a mysterious outbreak of juvenile rheumatoid arthritis near the community of Lyme, Connecticut. The rural location of the Lyme outbreak and the onset of illness during summer and early fall suggested that the transmission of the disease was by an arthropod (insect) vector.
In 1982, the cause of Lyme Disease was discovered by Willy Burgdorfer, who isolated bacterial spirochetes belonging to the genus Borrelia from the guts of Ixodes ticks. He showed that these spirochetes reacted with immune serum from patients that had been diagnosed with Lyme Disease. Subsequently, the bacteria was given the name Borrelia burgdorferi. Since then, reports of Lyme disease have increased dramatically to the point that the disease has become an important public health problem in some areas of the United States. Today, Lyme Disease is the most prevalent tick-borne illness in the United States.
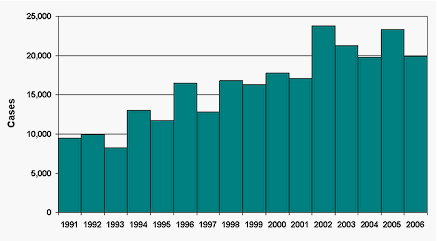
Incidence of Lyme Disease in the United States, 1991-2006.
|
From 1991 to 1994 there were less than 10,00 new cases per year reported to the CDC (Center for Disease Control). Between 1996 and 2001 the average number was about 17,000 new cases per year but increased to near or above 20,000 new cases per year in 2002. In 2006, there were 19,931.
Since 2002 there has been a repeated 100% increase
each year from the 1991 new cases per year averages. |
Lyme Disease is most commonly transmitted by a tick bite (usually painless). The tick vector (click here for images of different tick species) include but are not limited to, Ixodes scapularis (Deer Tick), Amblyomma americanum (Lone Star Tick) and Ixodes pacificus (Western Black Legged Tick). Ixodes dammini was once thought to be the only species responsible for transmission until it was shown to be the same as Ixodes scapularis in 1993. The Deer and Lone Star ticks can be found in many areas. The ticks prefer to live in wooded areas, low growing grassland, seashores and yards. Depending on the location, anywhere from less than 1% to more than 90% of the ticks are infected with the spirochetes that cause Lyme Disease.
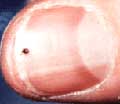 An example of an immature Deer tick compared to the size of an adult human's thumb
An example of an immature Deer tick compared to the size of an adult human's thumb
|
|
The most notorious of the tick species that transmit Lyme is the Deer tick. Not only are they tiny and difficult to detect, they also have a distinctive growing period that makes them especially dangerous for Lyme transmission.
The Deer tick has a 2 year life cycle where it must feed 3 times so that it can grow and reproduce. The first feeding occurs In the larvae stage, when it is tan, the size of a pin head and generally feeds on small animals like the mouse where it can pick up the spirochete. Having fed once, it grows and enters the nymph stage where the tick is the size of a poppy seed, beige or partially transparent and feeds on larger animals such as cats, dogs and humans. From that second feeding, it finally matures into the adult tick. This is when they are black and/or reddish and feed on cattle, deer, dogs and humans. Once the adult female tick has fed that third time, she is ready to mate and reproduce to continue the tick cycle. As the pictures show, ticks can be very difficult to see and tell which species is which. A quick way to identify the female Lone Star tick which is also a carrier of Lyme, is to look for it to have a grey body with a white dot on its back.
While April through October is considered the "tick season", Lyme disease can be transmitted at any time. Ticks are extremely active in the spring and early summer but Deer ticks are found year round including wintertime. So make sure to remember that a bite from a tick can happen at any time, not just the warm months of the year.
LOCATION
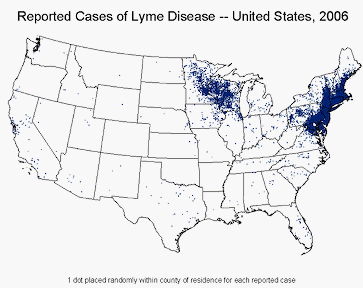 |
Cases of Lyme disease in the U.S. have been reported in virtually every state, although the Northeastern, Great Lakes, and Pacific Northwest areas are particularly endemic.
• In the northeastern states from Maine to Maryland
• Two north central states (Minnesota and Wisconsin)
• In the northwest (California and Oregon)
Lyme disease is also a serious problem around the world wherever there are ticks. The disease is common in Europe, particularly in forested areas of middle Europe and Scandinavia. The Borrelia family is also responsible for tick infections in Europe, but different subspecies ( B. garinii and B. afzelii) may be more common there and cause slightly different symptoms. The infection has also been reported in Russia, China, and Japan.
SYMPTOMS
Lyme disease is called the "Great Imitator" because it can mimic many other diseases, which makes diagnosis difficult. Many Lyme patients were firstly diagnosed with other illnesses such as Juvenile Arthritis, Rheumatoid Arthritis, Reactive Arthritis, Psoriatic Arthritis, Infectious Arthritis, Osteoarthritis, Fibromyalgia, Raynaud's Syndrome, Chronic Fatigue Syndrome, Interstitial Cystis, Gastroesophageal Reflux Disease, Fifth's Disease, Multiple Sclerosis, scleroderma, lupus, early ALS, early Alzheimers Disease, crohn's disease, ménières syndrome, reynaud's syndrome, sjogren's syndrome, irritable bowel syndrome, colitis, prostatitis, psychiatric disorders (bipolar, depression, etc.), encephalitis, sleep disorders, thyroid disease and various other illnesses.
Some people develop symptoms very soon after being bit by a tick. However, some people who have the disease do not develop symptoms until quite some time after the disease causing bite. In some cases, it may take years for any symptoms to show at all. Symptoms may also slowly reveal themselves over a long period of time with patients showing up at their doctors with vague, varied symptoms and no knowledge of a tick bite or rash. A bite from a very young tick that is very small may not leave a rash or a bite mark. There are even some people who have been exposed but may never develop Lyme symptoms. At this point, it's not yet known even how long the bacteria may lie dormant.
The most well known symptom of Lyme Disease is a rash at the site of the bite. A rash can appear several days after infection, or it may not develop at all. Only about 30% of people infected develop the tell-tale 'bulls-eye' rash (erythema migrans) from a tick bite, and even then, physicians often miss it. If it does develop, it can last a few hours or up to several weeks. It can look like a classic rash or it can look more like an allergic welt (click here for images of different Lyme rashes). The rash can be very small or very large (up to twelve inches across).
The "bullseye" rash is generally a round ring with central clearing. Unfortunately, this is not the only rash associated with Lyme. Various other rashes associated with LD have been reported. One bite can cause multiple rashes. The rash can mimic such skin problems as hives, eczema, sunburn, poison ivy, flea bites, etc. The rash can itch or feel hot or may not be felt at all. The rash can disappear and return several weeks later. For those with dark skin the rash will look like a bruise. If you notice a rash, take a picture of it. Some physicians require evidence of a rash before prescribing treatment.
Early Symptoms: Several days or weeks after a bite from an infected tick, a patient usually experiences "flu-like" symptoms such as aches and pains in their muscles and joints, low grade fever, and/or crushing fatigue.
Other Possible Symptoms (not a complete list) -- No organ is spared:
|
Head - |
uexplained hair loss
|
|
Jaw - |
pain in the teeth, chewing muscles and/or jaw joint, stiffness of the jaw, difficulty chewing, lock jaw, symptoms of TMJ (Temporal Mandibular Joint Disorder)
|
|
Bladder - |
frequent or painful urination, repeated cystitis (urinary tract infection), bladder nerve damage, incontinence (inability to control bladder)
|
|
Lung - |
respiratory infection, cough, asthma, pneumonia, painful breathing due to rib soreness
|
|
Ear - |
pain, ringing/tinnitus, sensitivity to noise, hearing loss
|
|
Eyes - |
pain due to inflammation, sensitivity to light, floaters (spots in front of the eyes), drooping of the eyelid, conjunctivitis (pink eye), blurring or double vision, vision loss caused by inflammation of the optic nerve (optic neuritis) and/or brain inflammation/swelling
|
|
Throat - |
sore throat, swollen glands, cough, hoarseness, difficulty swallowing
|
|
Neurological
/Brain - |
headaches, facial paralysis, seizures, meningitis, stiff neck, lower back/neck pain, burning, tingling, or prickling sensations, stabbing sensations, numbness, tremors or unexplained shaking, muscle twitches, tics, hand tremor, dizziness/vertigo, poor balance, increased motion sickness, loss of reflexes, loss of coordination, difficulty walking, MS like syndrome, peripheral neuropathy or partial paralysis, difficulty speaking or understanding speech
|
|
Stomach & Intestine - |
pain, diarrhea, nausea, vomiting, abdominal cramps, acid reflux, GERD, anorexia, irritable bowel syndrome (IBS)
|
|
Heart - |
weakness, dizziness, irregular and/or forceful beating of the heart (palpitations), rapid/fluctuating heart rate (tachycardia), slowing of the heart rate below 60 bpm (bradycardia), myocarditis (inflammation of the muscular walls of the heart), pericarditis (inflammation of the membrane surrounding the heart), transient heart blocks (the delay or complete inability of an electrical impulse to reach the correct area in the heart to make it pump blood), enlarged heart, heart valve damage, heart murmur, fainting, shortness of breath, chest pain, rib soreness
|
|
Joint - |
arthralgias (joint pain), arthritis (joint damage), joint swelling (particularly in the knees), muscle inflammation and pain, whole body muscle pain, migratory joint and muscle pains with or without objective signs of joint swelling, marked joint and muscle stiffness, tennis elbow, abnormal muscle fatigue, localized and widespread muscle spasms |
|
Other Organs - |
swollen body glands, liver infection, elevated liver enzymes, enlarged spleen, swollen testicles, irregular or ceased menstral periods
|
|
Neuropsychiatric - |
mood swings, irritability, hallucinations, psychotic episodes, poor concentration, cognitive loss, memory loss, confusion, stammering, loss of appetite, mental deterioration, depression, disorientation, sleep disturbance
|
|
Pregnancy - |
miscarriage, premature birth, birth defects, stillbirth
|
|
Skin - |
single or multiple rash, hives
|
|
General
Well Being - |
unexplained fevers (high or low grade), continual infections (sinus, throat, chest, etc.), low body temperature, allergies & chemical sensitivities, increased affect from alcohol and possible worse hangover
|
The above is a list of possible symptoms. Other symptoms not listed may also be present. They can occur in any combination. You may have one or several symptoms but not everyone will experience every symptom. Lyme affects each host in a different way. Having one or many of these symptoms does not indicate that you have Lyme disease. Diagnosis for Lyme is a clinical one and must be made by a physician experienced in recognizing LD.
TESTING
ELISA & IFA TEST
A variety of tests are available. Many doctors who are unfamiliar with Lyme disease may just use the Lyme test available in their local laboratory. The most common used are the EIA, the ELISA (often called "Titer Test”), the IFA or the PCR-DNA probe test. One of these tests will generally be the first line of testing used by the average doctor who suspects Lyme. The ELISA and IFA tests measure a patient's antibody, IgM and/or IgG, in response to exposure to the Lyme bacteria. These are usually done with blood drawn from the patient but may also be done on fluid from the spine or from a joint.
It may take up to 2 months after becoming infected before antibodies can be detected in a blood test. Once formed, antibodies usually stay in your system for many years, even after successful treatment of the disease. Finding antibodies to the Lyme disease bacteria does not tell whether you were infected recently or sometime in the past.
Antibody testing is generally done in a two-step process, using either the ELISA or IFA followed by the Western blot test. ELISA is considered a more reliable and accurate test than IFA, but IFA may be used if ELISA is not available. The Western blot test (which is a more specific test) should be done in all people who have tested positive or borderline positive (equivocal) in an ELISA or IFA test.
While the ELISA test is more reliable than the IFA, in and of itself, it is not very reliable at all. If the patient is not producing antibodies (either too early or later in the disease), false negatives may occur. Current ELISA tests have an estimated 65% failure rate of correctly detecting Lyme infections. One of the leading laboratories that tests for Lyme, IGeneX, Inc., will only perform the ELISA test when Western Blots are ordered in conjunction.
Unfortunately, while these tests are not very accurate when it comes to detecting Borrelia burgdorferi infection, many physicians who have not familiarized themselves with their high failure statistics, take them as being a definitive diagnosis source. Consequently they will tell their patients they do not have Lyme disease based solely upon results from these tests when in fact, that patient may very well have a case of Lyme that was not correctly detected. If utilizing a first line test, the PCR is considered the most reliable and may be a better option over the ELISA or the IFA.
WESTERN BLOT TEST
The Western Blot tests (IgG and/or IgM) are much more sensitive and specific than the above ELISA tests. With the Western blot, the laboratory can visualize the exact antibodies you are making to the Lyme bacteria. In some cases the laboratory may be able to say that your “picture of Lyme antibodies” is consistent with early disease or with persistent/ recurrent disease. Not all patients have antibodies at all times when tested. Antibodies are more commonly detected within the first year after infection, although re-infection may cause a significant rebirth of antibodies. At most, only 70% of patients have antibodies early, and the presence of antibodies alone does not make a disease diagnosis. While this is a much more sensitive test to detect the bacteria, it also can have reliability problems if it is not done correctly. Never the less, it may still be the best tool in diagnosing Lyme Disease.
LYME DOT BLOT ASSAY (LDA)
The Lyme Dot Blot Assay (LDA) looks for the presence of pieces of the Lyme bacteria in urine. The LDA has been useful in some patients with clinical symptoms and clinical history consistent with Lyme disease, who consistently test negative with antibody tests for Lyme disease.
POLYMERASE CHAIN REACTION (PCR)
The PCR (Polymerase Chain Reaction) test detects the presence of the DNA of the Lyme bacteria. PCR tests have more sensitivity early in the disease before patients have received antibiotics. The best specimen to test has not been defined. The test is usually performed on whole blood, serum, urine, CSF, or miscellaneous fluids/tissues.
QUANTITATIVE RAPID IDENTIFICATION OF BORRELIA BURGDORFERI (BOWEN Q-RIBB)
Bowen Q-RiBb (Quantitative Rapid Identification of Borrelia Burgdorferi) - A new testing method, that potentially represents a major breakthrough, is the Q-RiBb test, which has now been approved a US patent. Developed by Jo Anne Whitaker, M.D., a prominent international medical researcher, and Lyme disease patient, the Q-RiBb test is unique in its approach and potentially offers much greater accuracy than conventional testing. The method uses a fluorescent antibody technique on whole blood. As it is "quantative", the test can determine the extent of infection and may therefore be able to distinguish the carriers from the patients with serious disease. Another advantage is the brief time required to complete the test. A preliminary report of the findings is provided within 24 hours of receiving the specimen and the final report includes digital photographs of the findings. Finally, the Q-RiBb is the only test that is unaffected by whether the patient is currently (or recently has been) taking antibiotics.
FLOW CYTOMETRY
Flow Cytometry - This is the test that Central Florida Research Inc is now using to test for Borrelia burgdorferi infection and Lyme disease. It is considered by many to be the "gold standard" of diagnostic testing at present. The test is essentially a refinement of the Q-RiBb and is such is much more accurate than the Western Blot, and of course the other screening methods. The Central Florida Research Inc website states that a "A Borrelia burgdorferi fluorescent antibody is used to detect the antigen in whole blood. The test is set up manually and read by Flow Cytometry. The Flow Cytometer can count the number of organisms in 100,000 events in 2 minutes and 50,000 in 1 minute. To visually count the organisms in 100,000 events or 50,000 events using a microscope would be almost an impossibility. The Flow Cytometer counts the number of all events passing through the aperture and enumerates the organisms that react with the antibody. The test result will be reported as a percent of the counted events." Essentially this statement is explaining that the Flow Cytometry test is quantitative and is able to detect the severity of infection rather than simply giving a positive or negative result for the presence of Bb. For more information visit the Central Florida Research Inc website.
ERYTHEMA MIGRANS BIOPSY
If erythema migrans rash is present then a biopsy should be carried out as soon as possible. If Borrelia burgdorferi is present then it can be cultured from a tissue biopsy. This procedure can give a crucial early diagnosis of Lyme disease many weeks before antibodies will show up on many of the commonly used laboratory tests.
WHICH TEST IS BEST?
Lyme Disease is very complicated to diagnose because:
| • |
Lyme bacteria are not always detectable in the whole blood, even in active disease. The bacteria like to hide.
|
| • |
Medications taken for other ailments and pre-existing conditions can interfere with the tests.
|
| • | Every patient responds differently to an infection.
|
| • | Antibodies may only be present for a short time and at certain times in the stages of the disease.
|
| • | For patients with clinical symptoms of Lyme Disease who test negative by the IgG or IgM Western Blot, the Whole Blood PCR or the LDA/Multiplex PCR Panel on urine may be appropriate. There are physician-developed antibiotic protocols to enhance the sensitivity of the LDA. In addition, there seems to be increased sensitivity of this test during the start of menses.
|
No matter which test is used, false positives and false negatives do occur. Diagnosis should not be made solely by test results.
TREATMENT
Lyme Disease is treatable although the results of the disease ravaging the body may be permanent. Antibiotics are recommended for a minimum of four to six weeks. More chronic cases may require a longer treatment or repeated treatments. Treatment is either oral or intravenous. Those diagnosed later or have developed more serious symptoms may need to be treated with multiple weeks/months of I.V. antibiotics.
There are a wide range of treatments depending on the severity and stage of the disease. No one treatment is best although some are better than others. Chronic Lyme treatment is a controversial topic and requires monitoring and adjusting along the way to successfully combat the disease and the many symptoms associated with it. There is great debate as to whether a person is actually cured after treatment or is more along the lines of a person with Herpes that can go into remission until the immune system is stressed and then it resurfaces again.
Depending upon your treating doctor and what you feel most comfortable with, some people opt for a strictly Western Medicine approach while others incorporate holistic and alternative treatments in addition to the antibiotics. It is a personal choice as to which the patient prefers and what works best for them. The most important thing to remember though is to use common sense and beware of treatments which may make things worse. Even if it may seem overwhelming and mind numbing to try to understand how a treatment works, it's always best to know what's being done to you. Afterall, you're the one that has to live with the consequences!
If caught early, Lyme Disease is fairly easily treated with minimal problems. Unfortunately, delays in diagnosis and lack of appropriate treatment make getting rid of the disease much more difficult and allows it to do more damage to the body... with sometimes permanent and devastating results. Prompt attention and medical intervention can mean the difference between a quick recovery or a long and debilitating illness. In some instances, treatment may even mean the difference between life and death. If you feel that you may be infected, get yourself thoroughly checked and remember that a test is not a definitive diagnosis by itself. Find a doctor that will look at the whole picture, not just a test result.
As a general rule, when in doubt, seeking treatment is advised if:
You are bitten by a tick that tests positive for spirochetes
You are bitten by a tick and you have symptoms
You are bitten by a tick and are pregnant
You are bitten by a tick and live in an endemic area
LYME DISEASE PREVENTION
I. The best way to prevent Lyme Disease is to check frequently for ticks.
A. Check all body parts that bend including:
1. behind the knee
2. between fingers and toes
3. underarms
B. Check other areas where ticks are commonly found including:
1. belly button
2. in and behind the ear
3. neck
4. hairline
5. top of the head
C. Check pressure points including:
1. where underwear elastic touches the skin
2. where bands from pants and skirts touch the skin
3. anywhere else where clothing presses on skin
D. Go back and visually check all other areas
E. Run fingers gently over skin. If there is a tick and it is attached, it will feel like the last piece of scab left before a cut completely heals.
II. Shower after all outdoor activities are over for the day. If the tick is still wandering it may wash off.
III. If a tick is found, remove it carefully with fine tweezers. Grab as closely to the skin as possible. Do not squeeze the body, apply Vaseline, use a burnt match, or clean with alcohol while the tick is attached. Any of these actions could cause transmission of the bacteria.
IV. Ticks can be tested. Place tick in a glass or plastic vial with a moistened cotton swab. A clean pill vial is good. If none is available, use a ziploc storage bag as a temporary container.
V. Many Lyme Disease organizations now recommend prophylactic treatment when a person is bitten by a Deer tick in a known endemic area. Since there isn't enough evidence on either side to prove or disprove this theory, the final decision is up to the individual and the treating physician. The recommended treatment is 4-6 weeks of an oral antibiotic. Anyone needing information supporting treatment for a tick bite can obtain it by contacting the Lyme Disease Network.
VI. The use of sprays is a personal decision so you must know the facts. Products that contain DEET are tick repellents. They do not kill the tick and are not 100% effective in discouraging a tick from feeding on you. Products like Permanone contain premethrin and are known to kill ticks. However, they are not to be sprayed on the skin. Permanone can be sprayed on clothing. Once it is dry it is assumed to be safe. Ticks are anti-gravitational. They are generally seeking the highest point. If they get on your body below the clothes line, one hopes they will travel up and die once they come in contact with treated clothing.
Note: If the tick meets resistance on its journey to the top of your head it will stop and feed at that point. If you are wearing shorts and the tick gets stuck in the bend behind your knee the Permanone will not be helpful.
VII. Lyme Disease is a 12 month problem. The best defense against LD is education.
Lyme Disease symptoms vary from person to person. (lymes disease lyme's disease lime disease limes disease). The data and information presented in this web site are presented in good faith and believed to be accurate regarding Lyme disease (commonly misspelled lymes disease lyme's disease lime disease limes disease) and other related diseases. Any and all liability for the content or any omissions including any inaccuracies, errors, or misstatements in such data or information is expressly disclaimed. The web site is compiled for the sole purpose of informing community members of resources and information pertaining to Lyme Borreliosis Disease. Please consult a qualified Lyme ( Borreliosis ) Disease literate doctor for medical advice if Lyme Disease is suspected to discuss your Lyme Disease Symptoms.
|



